Our Technology
IntraLase™ FS Laser System
Allegretto WaveLight
Corneal Topography - Oculus Pentacam
Ocular Coherence Tomography (OCT)
Visual Field Testing - Perimetry
Frequency Doubling Technology (FDT)
Pachymeter
Digital Retinal Camera
Laser Therapy – Argon and YAG Lasers
Ultrasound A-Scan
The Zeiss IOL Master
IntralaseTM FS Laser System

Increasingly, successful LASIK procedures have one thing in common - they use AMO's IntraLaseTM FS Laser System.
At a nearly unprecedented level, LASIK has become a trusted way for people to improve their functional vision. And judging by the numbers, the IntraLase Method, using AMO's IntraLaseTM FS Technology, has become an integral part of today's advanced LASIK procedure. With well over 1 million procedures completed to date, IntraLaseTM FS Technology is clearly integral in improving the safety and accuracy of LASIK procedures.
Precision Technology For A Safer LASIK Experience: By replacing the blade commonly used for corneal flap creation with a femtosecond laser, AMO® has made LASIK eye surgery safer than ever before. The IntraLaseTM FS Laser System delivers micron-level accuracy 100% greater than a microkeratome for more accurate and consistent flap thickness - which is critical for a successful LASIK outcome.
Retrospective analysis comparing LASIK results with IntraLaseTM FS Technology versus the two leading microkeratomes demonstrated that IntraLaseTM FS Laser System performed better in three areas important to LASIK results and safety: flap thickness, induced astigmatism, and cell injury.
There are fewer flap-related complications with the IntraLase Method:
- Minimal risk of sight-threatening events (free caps, globe penetration, buttonhole flaps, decentered flaps, and/or incomplete cuts)
- No risk of corneal abrasion
- Reduced risk of dry eye
Allegretto Wavelight Laser

The Allegretto WaveLight Laser is a revolutionary approach to laser vision correction. The Allegretto WaveLight virtually eliminates night vision reduction, glare, and halos. It is fitted with a department-of-defence calibre eye tracking system.
The Allegretto WaveLight utilizes PerfectPulse Technology, which accounts for the laser's speed, precision, and safety. The smart energy control measures and adjusts energy levels in the laser pulse from creation to delivery. This control charts the eye's movement 200 times per second.
Every 4-6 milliseconds, the eye's location is measured and the internal mirrors of the Allegretto WaveLight are automatically aligned. Immediately before the pulse is released, a second check is made to confirm that the eye has not moved. This occurs 200 times per second, once for every laser pulse released. If the eye moves too quickly to be measured or moves out of range, the laser stops and will not let out another pulse until the eye is back in the proper position.
Unlike other laser correction systems, the Allegretto WaveLight adjusts to the patient's individual eye curvature. The Allegretto WaveLight sends extra pulses to the peripheral cornea, which compensates for the angle of the laser. The result is a smooth, effective optical zone.
The Allegretto WaveLight is capable of producing the largest possible optical zone of any lasers. If a patient's pupil is larger than the optical zone, they may experience poor peripheral vision, poor night vision, and a higher than normal incidence of halos and glare.
The Allegretto Laser is used for LASIK and other laser eye surgery procedures.
Corneal Topography - Oculus Pentacam
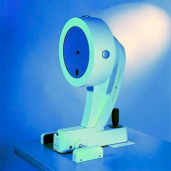
OCULUS PENTACAM - The Gold Standard in Anterior Segment Tomography/topography. Equipped with automatically rotating Scheimpflug cameras the Pentacam performs a complete measurement of the anterior eye segment in less than 2 seconds. A precise analysis of the central cornea is carried out in the process. During measurement extraneous eye movements are detected with a second pupil camera and automatically corrected during the calculation process. The software analyses and evaluates all the data acquired. These data then provide the basis for a three-dimensional model of the complete anterior eye segment.
The Pentacam analyses the entire cornea, anterior chamber and crystalline lens. The topographical map and computerised analysis reveals any distortions of the cornea, such as is keratoconus or corneal scarring, as well as the corneal curvature and meridians of astigmatism.
This diagnostic procedure is essential for patients being considered for refractive surgical procedures (such as LASIK) and may even be necessary in the follow-up of some patients who have undergone refractive surgical procedures. Many of our cataract patients also have this performed to confirm their eye measurements. Measurement is non-contact and entirely agreeable to the patient.
Ocular Coherence Tomography (OCT)
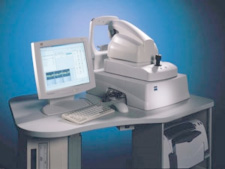
OCT is a new diagnostic tool that provides images of the back of the eye of unprecedented quality. This information is particularly helpful for diagnosing and monitoring many cases of retinal disease, as well as glaucoma, which previously had mystified even the most experienced clinicians.
OCT uses a principle akin to ultrasound. A beam of light is split in two, with one beam 'the reference' bouncing off a mirror a known distance away while the second passes through the pupil and is reflected off the various layers of the retina. OCT is 10 times more sensitive than ultrasound, with the ability to display objects as small as one hundredth of a millimetre wide. Unlike fluorescein angioography, previously the standard test for retinal disease injections which required the injection of a contrast dye and a very bright light, OCT is much easier to have done.
OCT is helpful not just for diagnosis but also for monitoring responses to treatment. It is, for example, invaluable in assessing both the suitability and the response to treatment of patients with diabetic retinopathy. OCT is now almost mandatory for the management of "wet" macular degeneration with the new "anti-VEGF" drugs Lucentis and Avastin which are given by injection into the eye every 4-6 weeks. These treatments are very effective but we try to limit their use because we suspect they may have long term side effects if they are given too often. OCT is used to confirm that treatment has been effective by making sure there is no bleeding or swelling left. Once treatment is stopped after the macula has settled, OCT examinations are performed regularly to check for recurrence.
Visual Field Testing - Perimetry

Most patients complain that they do not like doing field tests, but they are important for monitoring the disease. The shape of glaucoma blind spots tends to be curved or "arcuate" which corresponds to the distribution of the nerve fibres that are damaged. The defects usually start in the mid periphery. Ultimately when superior and inferior arcuate defects join up the patient is left with tunnel vision. When we test distance vision using a visual acuity chart with letters in rows we are only testing central vision, a patient can have perfect central vision till very late in glaucoma.
Our conventional approach of looking for visual field defects is with subjective white-on-white automated perimetry where the patient is asked to detect small light targets projected into their peripheral field of view. While some subjects are very good at field tests, we recognise that they are difficult and performance can be variable. This has to be taken into consideration when interpreting the result.
Frequency Doubling Technology (FDT)

Frequency Doubling Technology works by flickering a coarse pattern of vertical dark and bright bars at a very high frequency. This produces the appearance of twice as many bars than are physically present. The advantages of the FDT are that it is a compact, transportable perimeter with tolerance to refractive errors and rapid test times (less than 4 minutes per eye). In some cases it shows defects before they are seen on standard tests. It is very useful for visual field screening in the community.
Pachymeter

It has recently been determined that the thickness of an individual's cornea can influence the pressure reading and lead to under or over-estimates. For this reason we now perform Ultrasound Corneal Pachymetry on all our glaucoma patients as a baseline, to determine corneal thickness. This test is simple, painless and takes a few seconds. Please let us know if you haven't had it done - it is very important for determining an accurate pressure.
Digital Retinal Camera
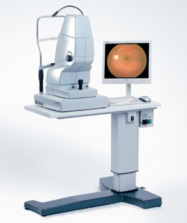
The Zeiss VisuCam is a state of the art retinal camera used for colour photography of the retina and optic discs as well as Fluorescein angiography (which is the standard investigation for macular disease).
Laser Therapy - Argon and YAG Lasers
There are now several possible applications for the use of lasers in the management of glaucoma and retinal conditions.
What is a Laser?
L.A.S.E.R. is actually an acronym for Light Amplification by Stimulated Emission of Radiation, and it is essentially a concentration of light energy into a narrow well focussed beam. What this beam does to the objects it comes into contact with depends on the "wavelength" of the light source. A wide variety of laser types exist, ranging from visible to invisible, and they are capable of heating, burning, cutting or disrupting, depending on the type and power combination selected. Their advantage in medicine is that they are extremely fine and can be accurately targeted.
The Argon Laser
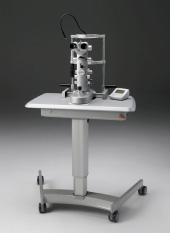
The Argon Laser is used for treating Retinal conditions and Glaucoma. Retinal tears can be surrounded by Laser barrier so they do not extend. Leaking blood vessels in Macular Degeneration and Diabetic Retinopathy are also treated with this Laser.
The YAG Laser

The YAG Laser is used to perform a posterior capsulotomy. This makes a hole in the posterior capsule of the lens, a thin residual membrane behind the implant lens which can become cloudy, usually several months to years after the cataract surgery has taken place.
It is also used to perform laser iridotomies, which are recommended in those patients at risk of angle-closure glaucoma. It prevents against this type of glaucoma by providing for a bypass for fluid within the eye.
Ultrasound A-Scan

An Axial Scan or A-Scan is an ocular ultrasound that accurately measures the length of your eye along the visual axis. A-scans are performed under a topical anaesthetic. The scanner head is placed directly onto the cornea to allow the sound waves to pass through the eye.
A-scans are used in the calculation of Intra Ocular Lenses (IOL) that are inserted in cataract surgery once the patient's natural lens has been removed. It is one of two vital tests that must be carried out before surgery.
The Zeiss IOL Master
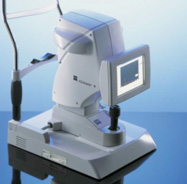
The Zeiss-Humphrey IOL Master is the first non-contact optical coherence biometer. This safe and effective laser system offers the most accurate and precise method of calculating a person's intraocular lens power. And it allows fast, accurate measurements of eye length and surface curvature, necessary for cataract surgery. The IOL Master is very efficient because it allows technicians to take all measurements with a high level of confidence in the accuracy of the results. Also, because it is non-contact (nothing touches the eye itself) there is no need for anaesthesia and there is no potential for spread of contamination from the instruments.
Specialist Eye Centre use this state-of-the-art technique for preoperative evaluation of the eye. As a back-up, we have a highly accurate ultrasound system which is more reliable in the presence of a dense cataract which obstructs the passage of light.
The IOL Master has been shown to increase measurement accuracy up to five-fold.
The information is then subjected to a range of sophisticated formulae which are gauged to best suit the individual eye so that an optimal outcome can be attained in each case.

